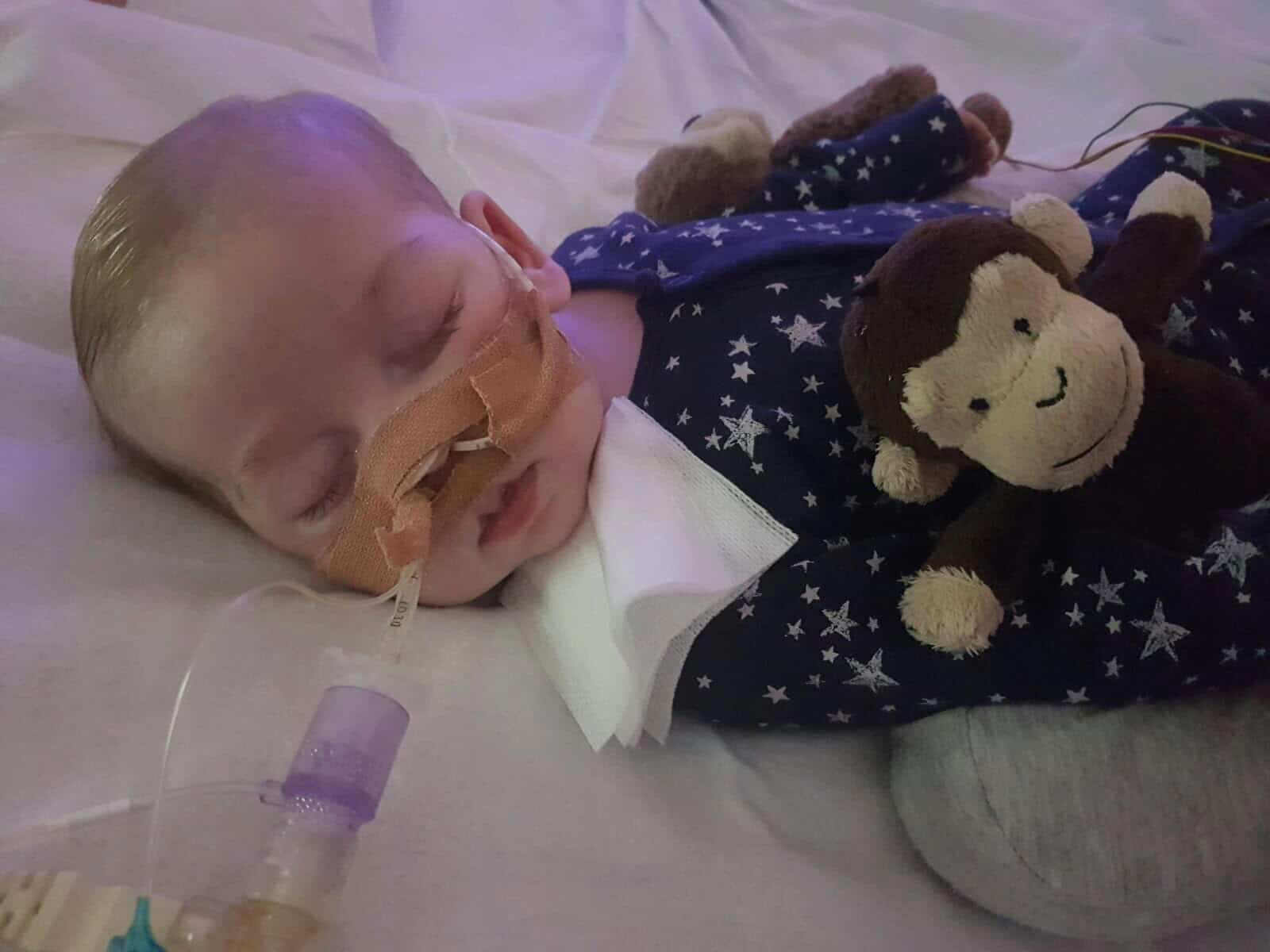
This past week my social media feed has been inundated with information about #CharlieGard. If you’ve missed out, here is a quick refresher:
10 month old Charlie Gard was born with a genetic mitochondrial disorder, infantile onset encephalomyopathic mitochondrial DNA depletion syndrome, or M.D.D.S. At this stage, it has placed him in need of life support. His parents started a GoFundMe to help get him to the USA for an experimental procedure yet to be tested on humans. The European Court of Human Rights (ECHR) has determined with the ethics board of the hospital, Great Ormond Street Hospital (GOSH), that it would be unethical, painful and dehumanizing to continue his life support, and that he should not be taken the United States.
Charlie’s condition is so rare that he is only the sixteenth reported case. The treatment may have as high as a 4% success rate. What is also uncertain is whether or not the experimental therapy will stop Charlie’s further deterioration or help him recover. As some have pointed out, his brain has so little function that a respirator is required for his breathing. It is also unknown if the experimental treatment, if successful, would improve his condition or allow his body to heal and repair itself. A Crux article mentions the recover of Arturito Estopinian, but it is unclear if he received the same treatment.
The case has even gone to the Vatican. Two statements have been made, one by the Pontifical Academy for Life and another from Pope Francis. As reported in the above Crux article, Pope Francis has asked if he could take in Charlie so he could receive medical care at the Vatican. The answer was an outright “No” by the ECHR. For the ECHR, this is not about money: it’s about ethics and allowing Charlie’s M.M.D.S. to run its course while he receives palliative care.
The case, however, continues to develop. New evidence has come forth that the experimental therapy treatment may be more successful than originally thought. GOSH and ECHR are willing to re-hear the case. If nothing else, this helps to show their good will, that they are not actively seeking to end Charlie’s life but, like his parents, hope for him to both live and die well. The events surrounding Charlie have been reminding me of my ministry as a hospital chaplain in the first months of my Jesuit formation.
***
I was standing next to him, a premature baby: John Doe – the parents weren’t read to name him yet. So small, in need of so much. I stood there with his mother, and we prayed silently together for his healing. I handed her a plastic rosary that the chaplaincy office had in multitude. We prayed an Our Father and Hail Mary. I moved to the next glass crib to pray over a child without a parent’s presence.
***
I am not a medical expert, nor am I a moral theologian. There are clear, strong arguments for the autonomy of Charlie’s parents. But there is also a case for the advice and opinion of the medical professionals, who have deemed it unethical to allow Charlie to continue a life of suffering when the odds of his survival are incredibly limited, and would rather allow him to die comfortably. Yet, parents do not have complete autonomy over their children: that’s why we have organizations such as Child Protective Services and require both adopting and foster parents to undergo extensive screening and check-ins.
There are conflicting rights: the right to the parent’s autonomy as care givers and the right of medical professionals to do no harm. But what if we spoke in the terms of Catholic Social Teaching? In particular, human dignity and the common good? Human dignity demands that Charlie deserves to be treated with a dignified life and death. Likewise, this value demands that all those involved in the decision making process, parents, doctors, judgets, be respected and heard. The value of the common good helps to clarify what specific actions need to be made. How might the community be affected by whatever decision is made? Monetary cost can never place the value of a human life, nor can a desire to experiment in order to help others if it would cause undue suffering on the person or they have not given consent. But what if there is also hope in a cure or treatment, or an opportunity to move closer to one?
***
I was asked to join the head of the chaplaincy office to the ICU floor of the hospital to witness something unfold. An elderly and very frail woman was lying in a hospital bed. The doctors asked if the head of the department could help convince her children to sign a DNR – Do Not Resuscitate – order. Maybe they would listen to a brother in a cassock rather than a white coat? He explained to them what aid could be given if her respiratory, cardiological, or kidney function failed, and what her quality of life would be like afterwards. Compressions would likely break her sternum, a breathing tube would make it impossible for her to be comfortable if she were not sedated, she would need dialysis or other invasive and painful treatments. A DNR order would ensure that if something happened, they could relieve her pain and let things run their course, they could donate her organs to save others’ lives. They agreed that this would be better.
A minute later we held a prayer service with the entire family now gathered in a once spacious-now cramped room. Each member of the family made the sign of the cross over their beloved mother, grandmother, great-grandmother. There was healing and hope for her and her family.
***
The rarity of M.M.D.S. and odds of the experimental therapy working may be the main point of contention within the greater question of conflicting rights. Is a 4% chance of success enough for hope? Of course it is. But we also have to be realists, and that makes me worry about how Charlie’s parents are being accompanied. Charlie’s parents are very much like the family members I encountered as a chaplain: they are clinging onto a sliver of hope, which does exist. As I imagine Charlie on life support surrounded by his parents, I also imagine the patients and family members I have met and prayed with, hoping for a miracle. But to what extent do we also need to be able to listen to medical and ethical resources at our disposal? I wonder what kind of pastoral care Charlie’s parents have been offered as they go through this process? How prepared are they to say good-bye, and who is helping to prepare them if it such a strong possibility? I can only begin to imagine the difficulty they are having in this moment.
In light of these questions, I have to ask myself how I can accompany others around me who face insurmountable odds and difficult decisions. How can I be an instrument of hope? For those times when an ethics board alone cannot help us, we all need some form of community for solidarity in sharing the joys and sorrows we experience. Whether it is a family struggling to determine how to proceed in the treatment of a sick family member, a person trying to find work for themselves and their family’s well-being, or a student struggling to pass exams, all of us experience a need for some kind of hope. We can respond by listening well to what is happening in their experience, offering both our presence and prayer – to be with them in love as they make their decisions.
With my hope that the Gard’s are making a well formed decision, it ultimately seems like it would be worthwhile for the hospital and ECHR to determine that any chance of survival as well as the possibility of an ethically sound experimental therapy is an act of hope in line with both Charlie’s and his parents’ dignity. If the therapy fails to treat him successfully, it will at least be a step forward to potentially helping the common good. Hopefully the entire community gathering around Charlie will be witnesses to him and his family of the importance of the human dignity of all in light of the common good.
***
Image courtesy Catholic News Service.